Introduction: The Rise of Wearable Sensors in Health Monitoring
The healthcare industry is increasingly leveraging technology to enhance patient outcomes, with wearable sensors playing a pivotal role in modern health monitoring. These devices provide continuous, real-time data on vital parameters such as heart rate, blood pressure, glucose levels, and activity patterns—insights that were previously difficult to obtain through traditional clinical methods.
The global market for wearable technology is expected to reach $74 billion by 2025, driven by advancements in sensor technology, increased demand for remote monitoring, and the rise of digital healthcare solutions. However, concerns about their accuracy, reliability, and regulatory compliance remain critical for their effective clinical integration.
This article examines the comparative accuracy of wearable sensors in clinical trials against traditional methods, exploring key themes, challenges, and opportunities. As these devices continue to evolve, ensuring data consistency and validation will be crucial in establishing their role as essential tools in healthcare and clinical research.
Understanding Wearable Sensors
Wearable sensors are advanced electronic devices designed to monitor various physiological parameters by being embedded in clothing, accessories, or directly worn on the body. These sensors track key health metrics such as heart rate, body temperature, activity levels, and more, offering real-time data that enhances personal health management and medical monitoring.
One of the primary advantages of wearable sensors is their non-invasive nature, allowing users to seamlessly integrate health tracking into their daily routines without discomfort or disruption. Their continuous data collection provides valuable insights for individuals managing chronic conditions, athletes optimizing performance, and healthcare professionals monitoring patients remotely.
As technology advances, wearable sensors are becoming more sophisticated, improving accuracy, battery life, and integration with digital health platforms. Their growing adoption highlights their potential to transform healthcare by enabling early disease detection, personalized treatment plans, and proactive health management, making them essential tools in modern medicine.
Traditional Clinical Measures: A Benchmark for Accuracy
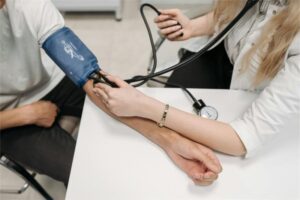
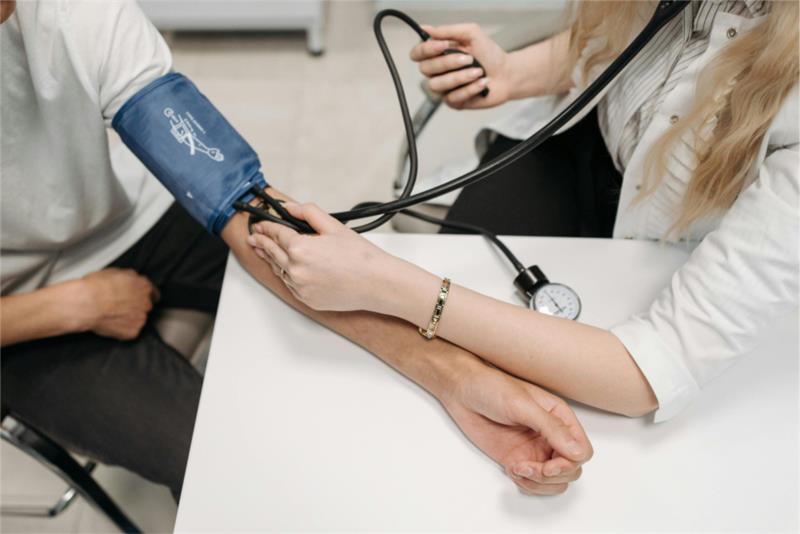
Traditional clinical measures serve as the foundation of medical diagnostics and patient monitoring, providing highly accurate and reliable data. These methods include blood pressure cuffs, electrocardiogram (ECG) machines, laboratory tests, and other standardized medical instruments widely used in hospitals and clinics. Their precision ensures effective diagnosis and treatment, making them the gold standard for evaluating new health technologies.
Key Aspects of Traditional Clinical Measures:
- High Precision and Reliability – Traditional methods are extensively tested and standardized, ensuring consistent and accurate health assessments.
- Controlled Testing Environment – Measurements are conducted by healthcare professionals in clinical settings, reducing external factors that may affect results.
- Limited Real-Time Monitoring – Unlike wearable sensors, these methods only capture health data at specific moments, making continuous tracking challenging.
- Benchmark for Wearable Devices – The accuracy of wearable sensors is compared to traditional methods to assess their clinical viability.
- Potential for Integration – Wearable sensors can complement traditional clinical tools, enhancing patient monitoring by providing real-time health data alongside established diagnostic methods.
Data Accuracy and Reliability in Wearables
The accuracy of wearable sensors compared to traditional clinical tools remains a subject of extensive research. While advancements in sensor technology have significantly improved the reliability of wearable devices, concerns about data accuracy persist. A study by the American Heart Association found that wearable devices can either overestimate or underestimate certain metrics, such as heart rate, by up to 10%. These discrepancies highlight the need for continuous validation to ensure wearables meet clinical standards.
Understanding the variations between wearable sensors and traditional medical devices is crucial for their broader adoption in healthcare settings. Factors such as sensor placement, user movement, and device calibration can all influence accuracy. Despite these challenges, wearables offer valuable real-time health insights that complement traditional clinical assessments.

Key Data Points on Wearable Accuracy
Metric | Traditional Measure | Wearable Sensor Accuracy | Discrepancy Range |
|---|---|---|---|
Heart Rate | ECG | 90-95% | 5-10% |
Step Count | Pedometer | 88-92% | 8-12% |
Blood Pressure | BP Cuff | 75-85% | 15-25% |
Although wearable sensors provide a convenient and non-invasive approach to health monitoring, their accuracy must continue to improve for wider acceptance in clinical environments. Ongoing research and technological advancements are key to minimizing discrepancies and enhancing their role in patient care.
Benefits of Wearables in Clinical Trials
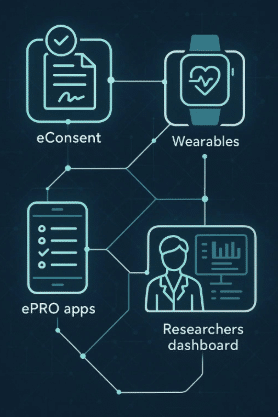
The integration of wearable sensors in clinical trials has transformed the way health data is collected and analyzed. These devices offer continuous, real-time monitoring, enhancing the accuracy and depth of patient data beyond what traditional clinical visits can provide. By capturing physiological parameters in real-world settings, wearables help researchers gain a more comprehensive understanding of how lifestyle factors influence health outcomes.
Key Benefits of Wearables in Clinical Trials
- Enhanced Data Quality – Wearable sensors provide continuous monitoring, reducing reliance on self-reported data and minimizing errors associated with infrequent clinical visits.
- Real-World Health Insights – Unlike traditional methods that capture data at specific points in time, wearables track daily variations in health metrics, offering a more holistic view of a patient’s condition.
- Improved Patient Adherence – Wearables simplify the data collection process, reducing the burden on participants and increasing compliance with study protocols.
- Facilitation of Decentralized Trials – Wearables enable remote monitoring, allowing trials to be conducted outside of clinical settings. This reduces logistical challenges, broadens participant demographics, and improves retention rates.
- Real-Time Data Transmission – These devices provide instant access to patient data, allowing researchers to detect trends, identify potential health risks early, and adjust study protocols as needed.
- By integrating wearable sensors, clinical trials become more efficient, cost-effective, and patient-centric. As technology continues to advance, wearables are expected to play an increasingly vital role in shaping the future of medical research and personalized healthcare.
Challenges in Wearable Sensor Adoption
While wearable sensors hold great promise for transforming healthcare and clinical research, their widespread adoption faces several challenges. Issues such as data privacy, variability in data accuracy, regulatory compliance, and system integration must be addressed to ensure their effectiveness and acceptance in medical settings.
Key Challenges in Wearable Sensor Adoption
- Data Privacy and Security – Wearable devices collect sensitive health information, raising concerns about data breaches, unauthorized access, and ethical considerations regarding patient consent. Strong encryption and regulatory frameworks are essential to protect user data.
- Variability in Data Accuracy – Differences in sensor quality, placement, and external factors like movement can affect the accuracy and reliability of wearable-generated data. Standardized testing and calibration are necessary to improve consistency.
- Regulatory and Compliance Barriers – The lack of clear regulatory standards across different regions makes it difficult for wearable devices to gain widespread clinical approval. Establishing guidelines for data validation, safety, and effectiveness is crucial.
- Interoperability with Healthcare Systems – Wearables generate vast amounts of data, but integrating this information with existing electronic health records (EHRs) and clinical workflows remains a challenge. Ensuring compatibility with healthcare infrastructure is key to maximizing their utility.
- User Adoption and Engagement – Patients and healthcare providers may be hesitant to fully adopt wearable technology due to concerns about accuracy, usability, and long-term benefits. Education and training can help improve trust and adoption.
Addressing these challenges will be vital for wearable sensors to become an integral part of healthcare, enabling better patient monitoring, disease management, and clinical research advancements.
Comparative Studies and Findings
Several studies have examined the accuracy and reliability of wearable sensors compared to standard clinical tools. Research has shown that while wearables offer promising results, their effectiveness depends on factors such as device quality, sensor placement, and patient compliance.
A study published in the Journal of Medical Internet Research found that wearable devices can predict health outcomes with an accuracy of 87% when compared to traditional clinical methods. However, the study also emphasized that variations in device quality and user adherence can impact the accuracy of collected data. This highlights the need for continuous validation and improvements in wearable technology to ensure their reliability in medical applications.
Comparison of Wearables and Traditional Methods
Evaluation Parameter | Wearable Devices | Conventional Methods |
|---|---|---|
Accuracy of Predictions | 87% | 95% |
Effect on User Compliance | High | Moderate |
Rate of Data Collection | Continuous | Periodic |
Variability in Reliability | Moderate | Low |
While wearable sensors provide real-time monitoring and enhance patient engagement, their integration into clinical practice requires ongoing validation and refinement. Standardizing accuracy benchmarks and ensuring regulatory compliance will be crucial for their broader acceptance in healthcare.

Future Prospects of Wearable Technology
As wearable technology continues to evolve, its capabilities are expected to expand significantly. Future advancements will focus on developing sophisticated algorithms for more accurate data interpretation, enhancing battery life for prolonged usage, and improving device design for better user comfort. These innovations will ensure that wearables not only complement but, in some cases, surpass traditional clinical tools in monitoring and diagnostics. With the integration of artificial intelligence and machine learning, wearable devices will become more efficient in detecting health anomalies, enabling early intervention and personalized treatment plans.
Industry Trends and Innovations
The wearable technology industry is experiencing rapid advancements, driven by AI-powered data analytics, nanotechnology, and smart sensors. A key trend is the incorporation of Advanced Biomarkers in wearables, allowing them to monitor complex health parameters beyond basic vitals such as heart rate and step count. This shift will significantly enhance their role in personalized medicine and preventive care, providing deeper insights into an individual’s overall health and potential risks.
Regulatory Considerations for Wearables
To ensure safety, efficacy, and reliability, regulatory bodies such as the FDA and other global health organizations are working on establishing standardized guidelines. These regulations will focus on data accuracy, patient safety, and the integration of wearable data with healthcare systems. As regulatory frameworks become more defined, the adoption of wearables in both clinical settings and home healthcare will expand, solidifying their role as essential tools in modern medicine.
Conclusion
Wearable sensors serve as a valuable complement to traditional clinical measures, offering continuous health monitoring and enhancing patient-centric care. Their ability to provide real-time insights has the potential to transform healthcare by improving disease management, clinical research, and personalized treatment strategies.
While challenges such as data accuracy, regulatory compliance, and integration with healthcare systems remain, ongoing advancements in technology and evolving industry standards are paving the way for broader adoption. As wearables become more sophisticated and reliable, their role in modern healthcare will continue to expand, bridging the gap between traditional diagnostics and digital health solutions.
The future of wearable technology is promising, with innovations in AI, biometrics, and remote monitoring set to revolutionize patient care and clinical trials. To stay informed on the latest advancements in wearable health solutions and decentralized clinical trials, visit Delve Health and explore how cutting-edge technology is shaping the future of healthcare.
Frequently Asked Questions
How accurate are wearable sensors compared to traditional clinical tools?
Wearable sensors are generally accurate, but their performance can vary by device and metric. Compared to traditional clinical tools like ECG machines and BP cuffs, wearables may fall short in precision by a margin of 5-25%. Factors such as device quality, user compliance, and data processing algorithms influence accuracy. Continuous improvements in technology are closing this gap, making wearables a viable supplementary tool in healthcare.
Can wearables completely replace traditional clinical methods?
While wearable sensors are increasingly sophisticated, they are not positioned to completely replace traditional clinical methods. Currently, wearables complement these methods by providing continuous monitoring and granularity that stationary equipment cannot offer. Traditional tools remain essential for acute diagnostics and treatments. Wearables, however, offer unparalleled data for preventive care and chronic disease management.
What challenges do wearables face in healthcare adoption?
Wearables face several challenges in healthcare adoption, including data privacy and security concerns, the need for standardized regulatory frameworks, and ensuring data interoperability with existing health systems. Variability in data quality between devices and user compliance also affects adoption rates. Addressing these challenges is critical for their successful integration into healthcare systems worldwide.
What role do wearables play in clinical trials?
Wearables significantly enhance clinical trials by providing continuous and real-time patient data. They facilitate decentralized trials, improve patient adherence, and allow researchers to capture lifestyle factors that can influence outcomes. These advantages lead to more comprehensive data sets and enable better-informed clinical decisions, making trials more efficient and cost-effective.
What are the future trends for wearable technology?
The future of wearable technology is marked by AI-driven data analytics, integration of advanced biomarkers, and enhancements in battery efficiency and design. These trends are likely to expand the role of wearables in personalized medicine and preventive care. Ongoing innovations point towards more reliable, accurate, and versatile wearables that will redefine patient care and health monitoring globally.